Common Tests During Pregnancy
Being pregnant means lots of trips to the hospital before your little one even makes an appearance. It may seem like you are being poked and prodded a lot, but every test is important and allows your doctor to track your baby’s growth.
ULTRASOUNDS:
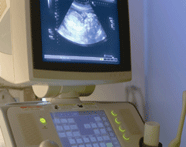
An ultrasound scanner is a machine that uses high-frequency sound waves to create an image of the internal organs (and your baby) on a monitor. Ultrasounds can be shown in 2, 3 or 4-dimensional images. You will undergo many ultrasounds during your pregnancy, each one for different reasons.
First Trimester: 0 – 12 weeks
At this early stage, the ultrasound can approximate your conception date and determine the number of fetuses by looking at the placenta. The doctor will also examine your pelvis, and check the fetus for any visible abnormalities.
Second Trimester: 13 – 27 weeks
This scan (sometimes called the “18-20 week scan”) looks at many things, including examining the placenta and observing the behaviour and growth of the fetus. The ultrasound will help deter-mine any abnormalities and assist with the amniocentesis test. The doctor will also look at the blood flow levels and amniotic fluid in the placenta.
Third Trimester: 28 – 42 weeks
These scans will determine the position of the fetus and measure the amniotic fluid level. The doctor will assess the growth and development of the fetus, as well as conduct a biophysical profile. The biophysical profile measures the conditions in the womb and the movements of the fetus. Scores of 8 – 10 are considered normal; anything below 6 is cause for concern.
GLUCOSE TOLERANCE TEST:
Third Trimester: 28 – 42 weeks
This test looks for gestational diabetes by testing the sugar / glucose levels in the mother’s blood. The mother is asked to drink only water on the day of the test. When she arrives for the exam, she is given a glucose solution to drink. Blood samples drawn over the next few hours measure the rate at which her body and the fetus break down the glucose. Gestational diabetes usually disappears after the birth of the child.
GROUP B STREP CULTURE:
35 – 37 weeks
Group B Strep culture is found in 30% of all women, and only becomes a complication when pregnant. GBS can cause severe illness in the mother during pregnancy, as well as pass bacteria (resulting in pneumonia, meningitis) on to the fetus as it is in the birth canal. Antibiotic treatment of mothers who have GBS greatly reduces the risk of transmitting infection to the infant.
BLOOD TESTS:
Throughout
Blood tests are conducted throughout the pregnancy, and are used to check for: blood type & antibodies, hemoglobin levels, Rubella vaccine, Hepatitis B, HIV, and syphilis.
URINE TESTS:
Throughout
Specifically, the urine is tested for levels of sugar and protein. Testing the glucose allows the doctor to see how glucose is being absorbed by the body. Testing the protein levels allows the doctor to notice high blood pressure, urinary tract infections and kidney disease.
The following tests are done to screen for birth defects:
CHORIONIC VILLUS SAMPLING (CVS):
10 – 12 weeks
This test involves taking a sample of the placenta, since the placenta contains the same genetic makeup as the fetus. Doctors use this tissue to test for abnor-malities in the genes. Knowing your family history comes in handy here – it allows doctors to screen more efficiently.
NUCHAL TRANSLUCENCY (NT):
10 – 14 weeks
NT tests are conducted at this time if there is a family history of genetic abnormality. An NT test examines the area at the back of the fetus’ neck for signs of abnormalities that can indicate Down’s syndrome, and heart defects. These tests are not 100% accurate; false positives and negatives can occur.
ALPHA-FETOPROTEIN (AFP) SCREENING TEST:
16 – 18 weeks
This is a blood test that determines pregnancies that are at a higher risk for birth defects like spina bifida or Down’s Syndrome. The liver of the fetus produces alpha-fetoprotein, which crosses the placenta into the mother’s blood stream. By testing the levels of AFP in the mother’s blood, the doctor can gauge the development of the fetus. An AFP test does not diagnose birth defects; instead, it can only indicate an increased risk. Like the NT test, false positives and negatives can occur. If an abnormality is detected, further testing (usually amniocentesis) is conducted…
AMNIOCENTESIS:
15 – 20 weeks
This test is common for women who are over 35 when they conceive. The doctor will withdraw fluid from the amniotic sac using a long thin needle. By testing the fluid, doctors will be able to see if there is an open neural tube defect, like spina bifida, and to analyze the genetic materials provided by cells in the fluid. Avoid strenuous activity for 24 hours after this procedure.




